Tuberculosis BCG vaccination
What is BCG?
BCG is a vaccine against tuberculosis (TB). It uses a live TB germ that has been modified in the laboratory so that it will not cause disease in a healthy person.
The BCG vaccination is not part of the WA routine vaccination program it is only given in restricted circumstances.
The BCG 10 Anti-Tuberculosis Vaccine is supplied as an unregistered therapeutic good under section 19(5) of the Therapeutic Goods Act 1989
How is the BCG vaccine given?
It is injected between the layers of skin on the upper arm near the shoulder by a Registered Nurse who has been trained in providing the vaccination.
Is the vaccine safe?
In most circumstances the vaccine is safe. As with any vaccination, BCG can result in severe adverse reactions and you should discuss this with the nurse before vaccination.
Are there any side effects?
Possible side effects include:
- Pustule or ulceration at site of injection
- Pain, redness and swelling around the injection site
- Swelling of the glands in the armpit and/ or neck
Rare side effects:
- Severe allergic reactions.
How effective is the vaccine?
- BCG vaccination reduces the risk of tuberculosis in people who are not already infected with TB. The vaccine does not always prevent disease.
- It is more effective in children < 6yrs old, providing 50 to 80 % protection against meningeal and miliary TB.
- Protection against TB will only start 6-8 weeks after the vaccination has been given and lasts for about 10 years.
- Revaccination is not recommended.
- BCG vaccination is not recommended for adults.
Who could be vaccinated?
- Children less than 6 years old who are;
Going to live in another country with a high incidence of tuberculosis (defined as an annual incidence of > 40 per 100 000 population) for more than 3 months or
- Will be making repeated visits to a country with a high incidence of tuberculosis that is likely to be for a cumulative period of more than 3 months.
For country specific incidence rates see the World Health Organisation TB country profile website (external site).
- Newborn children of migrants who have arrived from countries with a high incidence of tuberculosis (see definition above) in the last 5 years, or newborn children who have household contact with people who have arrived from a high incidence country in the last 5 years.
- Newborn children of parents with Leprosy or a family history of Leprosy.
- Children less than 6 years old who have not previously been vaccinated with BCG and are household contacts of newly diagnosed Leprosy case.
Who should not be vaccinated with BCG 10 Anti-Tuberculosis Vaccine?
- Infants with a body mass below 2,000g.
- Newborn children with suspected congenital immune deficiencies
- Persons who have had a tuberculin skin test (TST) reaction.
- Persons who have TB disease now, or have had TB disease in the past.
- Persons with HIV infection; including newborn children of mothers infected with HIV until this infection is ruled out in the child.
- Newborn children of mothers treated in their third trimester with medications such as anti-TNF-alpha monoclonal antibodies.
- Persons with primary or secondary immune deficiencies (including interferon-gamma deficiency and DiGeorge syndrome)
- Persons who take anti-cancer or steroid drugs such as cortisone or immunosuppressive drugs(including anti-TNF-alpha monoclonal antibodies such as infliximab) or are undergoing radiotherapy
- Patients after bone marrow stem cell transplantation or organ transplantation
- Persons who have had a serious illness such as kidney disease.
- Patients with malignant diseases (e.g. leukaemia, Hodgkin lymphoma, lymphoma, or other carcinoma of the reticuloendothelial system);
- Patients after bone marrow stem cell transplantation or organ transplantation;
- People with generalised skin diseases such as eczema or other exudative inflammatory dermatological conditions
- People with known hypersensitivity to any component of the vaccine.
- Pregnant women
- Persons with serious diseases (including severe malnutrition)
When should BCG vaccination be delayed?
- If another live vaccine (excluding oral Rotavirus) has been given within 4 weeks (measles, mumps, rubella, yellow fever, or varicella)
- Infection with a fever
- Generalised skin conditions
- Aggravation of a chronic disease
- Premature newborn children in an unstable clinical condition, until their general condition has improved
IMPORTANT INFORMATION POST VACCINATION
PLEASE KEEP THESE INSTRUCTIONS UNTIL THE SORE HAS COMPLETELY HEALED
What to expect after BCG Vaccination
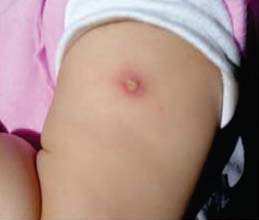
- BCG vaccination is given into the skin on the upper arm. Immediately after the injection a white lump is seen for a few minutes
- A red spot / small swelling will appear in 2– 4 weeks’ time
- This may develop into a pustule
- This pustule / lesion will heal spontaneously 2 – 3 months after vaccination. A scar usually remains at the site of the injection
What to do if a sore appears
- Leave the sore alone and ensure it remains exposed to the air. This helps it to heal quickly.
- Keep the affected site clean
What not to do
- Do not scratch, squeeze or disturb the sore or scab Do not apply ointment
- Do not apply antiseptics
- Do not apply sticking plaster or a tight sealed dressing as these can delay healing
- The child’s arm where the BCG vaccine has been administered should not be used for at least 3 months after the BCG vaccination for any other vaccines.
If your child experiences an adverse event after the BCG please report this to the Western Australian Vaccine Safety Surveillance (WAVSS) System (external site) Phone: (08) 6456 0208
Where can I get more information?
To request a booking for your child/children, please complete the BCG Vaccination booking request form:
Booking request form
Please ensure that you complete all the requested information on the form to allow for the booking to be completed.
After submitting the form, you will receive a confirmation email and an information sheet. You will then receive an appointment letter two to three weeks after receipt of form.
Your appointment will be at the WA TB Control program – located at Anita Clayton Centre 1/311 Wellington Street Perth.
If you have any questions please telephone the WA TB Control Program at the Anita Clayton Centre between 8.15am and 4.15pm Monday to Friday on 9222 8500 and request to speak to a nurse.
Last reviewed: 09-04-2024
Acknowledgements
Anita Clayton Centre (WA Tuberculosis Control Program)
This publication is provided for education and information purposes only. It is not a substitute for professional medical care. Information about a therapy, service, product or treatment does not imply endorsement and is not intended to replace advice from your healthcare professional. Readers should note that over time currency and completeness of the information may change. All users should seek advice from a qualified healthcare professional for a diagnosis and answers to their medical questions.